Primary ciliary dyskinesia is drawing renewed attention across the medical community as advances in genetics, diagnostics, and patient care continue to reshape how this rare condition is identified and managed. Long considered difficult to diagnose and even harder to treat, the disorder is now better understood than at any point in the past, offering clearer pathways for patients, families, and clinicians.
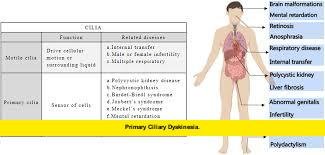
This inherited condition affects the function of motile cilia—microscopic, hair-like structures responsible for moving mucus, fluid, and particles out of the airways. When these structures fail to work properly, the result is a lifetime of respiratory challenges that often begin at birth and progress without targeted care.
If you or someone you care about has ongoing respiratory symptoms that never seem to resolve, paying attention to these developments may help you recognize when specialized evaluation is needed.
How Primary Ciliary Dyskinesia Affects the Body
Cilia line several vital areas of the body, including the nasal passages, sinuses, lungs, middle ear, and reproductive tract. In healthy individuals, cilia beat in a synchronized pattern that clears mucus and pathogens. In people with primary ciliary dyskinesia, this movement is absent, uncoordinated, or ineffective.
As a result, mucus accumulates in the airways, creating an environment where bacteria can thrive. Over time, this leads to chronic cough, frequent chest infections, persistent nasal congestion, sinus inflammation, and repeated ear infections. Many patients develop bronchiectasis, a permanent widening of the airways that makes infections more frequent and difficult to treat.
In about half of affected individuals, internal organs are positioned in a mirror-image arrangement, a condition known as situs inversus. While this does not usually cause symptoms on its own, it can be a critical diagnostic clue when combined with respiratory problems.
Why the Condition Is Often Missed or Diagnosed Late
One of the most persistent challenges with primary ciliary dyskinesia is delayed diagnosis. Symptoms frequently resemble those of more common conditions such as asthma, chronic bronchitis, or recurrent sinus infections. Because PCD is rare, many patients spend years receiving treatments that manage symptoms without addressing the underlying cause.
Newborns with the condition may experience breathing difficulties shortly after birth, yet the connection to a genetic ciliary disorder is not always recognized. Children often present with year-round nasal congestion, chronic wet cough, and hearing issues that persist despite standard treatment. Adults may not receive a diagnosis until significant lung damage has already occurred.
Earlier recognition allows for proactive management strategies that can slow disease progression and improve long-term respiratory outcomes.
The Expanding Role of Genetic Testing
Genetic research has transformed understanding of primary ciliary dyskinesia. Scientists have identified more than 50 genes involved in the structure and function of motile cilia. Mutations in these genes disrupt the mechanical processes that allow cilia to move effectively.
Genetic testing now plays a central role in diagnosis, especially when combined with clinical evaluation and specialized testing. Identifying the specific gene involved can help explain why symptoms vary widely among patients and may guide future treatment approaches as precision medicine evolves.
Researchers have also discovered that certain populations carry higher frequencies of specific gene variants, highlighting the importance of awareness and targeted screening in communities where PCD may be more common than previously assumed.
Advances in Diagnostic Techniques
Diagnosis no longer relies on a single test. Instead, clinicians use a structured approach that includes nasal nitric oxide measurements, high-speed imaging of ciliary motion, electron microscopy, and genetic analysis.
Low nasal nitric oxide levels are a strong indicator of PCD and are increasingly used as an initial screening tool. Advances in imaging technology allow specialists to observe cilia movement in real time, helping distinguish between structural defects and coordination problems.
Together, these tools improve diagnostic accuracy and reduce the number of patients who remain undiagnosed or misdiagnosed for years.
Current Treatment Strategies Focus on Prevention
There is currently no cure for primary ciliary dyskinesia, but treatment has become more effective at preserving lung function and reducing complications. Management centers on preventing infections, maintaining airway clearance, and monitoring disease progression.
Daily airway clearance therapy is a cornerstone of care. This includes physical techniques and devices that help loosen and remove mucus from the lungs. Prompt treatment of respiratory infections with appropriate antibiotics helps limit lung damage. Regular hearing evaluations and sinus care are also essential, particularly in children.
Specialized care teams play an important role, coordinating pulmonology, otolaryngology, physical therapy, and genetic counseling to address the full range of patient needs.
Research Moves Toward Targeted Therapies
Scientific momentum continues to build around therapies that address the root cause of the disease rather than symptoms alone. Laboratory models using patient-derived airway cells are allowing researchers to study how specific genetic mutations alter ciliary structure and movement.
These models are opening the door to gene-based approaches, including therapies designed to replace or repair defective genetic instructions. While these strategies remain under development, they represent a major shift in how PCD may be treated in the future.
Pharmacologic research is also exploring medications that may improve mucus clearance, reduce inflammation, or enhance residual ciliary activity, potentially improving daily respiratory function.
The Growing Importance of Clinical Trials
Clinical trials are becoming increasingly important in advancing care for people with primary ciliary dyskinesia. These studies evaluate new inhaled therapies, medications, and management strategies that aim to improve quality of life and slow lung disease progression.
Participation in clinical research helps generate the evidence needed to establish new standards of care. It also gives patients access to emerging therapies under close medical supervision.
As awareness of PCD grows, more trials are being designed specifically for this population rather than relying on data extrapolated from other respiratory diseases.
Quality of Life and Long-Term Outlook
Living with primary ciliary dyskinesia requires ongoing attention, but outcomes continue to improve as care becomes more specialized. With consistent management, many individuals maintain stable lung function well into adulthood.
Fertility challenges can occur, particularly in males, due to the role of cilia in reproductive systems. Advances in reproductive medicine offer options for family planning, and early counseling helps patients make informed decisions.
Education, adherence to treatment plans, and access to specialized care remain key factors in long-term health and independence.
A Condition Gaining Long-Overdue Visibility
Greater awareness among healthcare providers and the public is changing the narrative around primary ciliary dyskinesia. What was once considered an obscure diagnosis is now recognized as a condition that benefits greatly from early detection and coordinated care.
Ongoing research, improved diagnostic tools, and expanding clinical expertise continue to narrow the gap between symptom onset and diagnosis. For patients and families, this progress brings clarity, validation, and hope for better outcomes ahead.
Join the conversation by sharing your thoughts or experiences below and stay connected as understanding of this condition continues to grow.