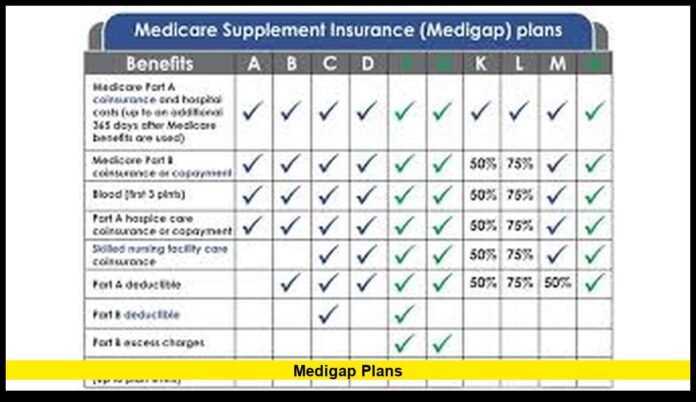
Medigap plans are gaining renewed attention in 2026 as rising Medicare costs lead many U.S. retirees to review supplemental insurance options that help reduce out-of-pocket healthcare expenses. Millions of Americans enrolled in Original Medicare rely on Medigap policies to cover deductibles, coinsurance, and copayments that Medicare Parts A and B do not fully pay.
Healthcare costs continue to climb, and adjustments to Medicare deductibles and premiums have made supplemental coverage an important financial planning tool. For many seniors, Medigap insurance helps create more predictable medical expenses during retirement.
Understanding How Medigap Plans Work
Medigap, also called Medicare Supplement Insurance, is private health coverage designed to work alongside Original Medicare. It fills many of the “gaps” in Medicare coverage by helping pay for expenses that beneficiaries would otherwise cover themselves.
Medigap policies may help pay for:
- Copayments
- Coinsurance
- Hospital deductibles
- Skilled nursing facility costs
- Certain medical expenses not fully covered by Medicare
When a beneficiary receives medical care, Medicare typically pays its share first. After that, the Medigap policy pays some or all of the remaining eligible costs, depending on the plan.
To purchase a Medigap policy, individuals must be enrolled in:
- Medicare Part A (hospital insurance)
- Medicare Part B (medical insurance)
Medigap policies cannot be used together with Medicare Advantage plans.
Medicare Cost Changes in 2026
Annual Medicare adjustments affect how much beneficiaries pay for healthcare. In 2026, several costs have increased, prompting more seniors to explore supplemental coverage.
Below is an overview of important Medicare costs for 2026:
| Medicare Expense | 2026 Amount |
|---|---|
| Part B monthly premium | $202.90 |
| Part B deductible | $283 |
| Part A hospital deductible | $1,736 |
| Prescription drug out-of-pocket cap | $2,100 |
These rising expenses highlight why many Americans choose Medigap policies to manage financial risk when unexpected medical needs arise.
Standardized Medigap Plan Options
Medigap plans follow federal standardization rules. Each plan type provides the same core benefits regardless of which insurance company sells it. The main difference between insurers is the price they charge for the policy.
The standardized Medigap plans include:
- Plan A
- Plan B
- Plan C
- Plan D
- Plan F
- Plan G
- Plan K
- Plan L
- Plan M
- Plan N
While benefits for each plan remain consistent nationwide, premiums can vary based on age, location, insurer pricing methods, and other factors.
Plan G Leads the Market for New Medicare Beneficiaries
Plan G has become the most popular option for many Americans who became eligible for Medicare after 2020. New beneficiaries cannot enroll in Plan F, which previously offered the most comprehensive coverage.
Plan G covers many important Medicare expenses, including:
- Hospital costs after Medicare benefits are used
- Hospice coinsurance
- Skilled nursing facility coinsurance
- Part B coinsurance
- Excess charges from certain physicians
The only major cost Plan G typically does not cover is the annual Medicare Part B deductible.
Because of this balance of coverage and cost, many retirees consider Plan G one of the most practical Medigap choices available today.
High-Deductible Medigap Options
Some policyholders choose high-deductible Medigap plans as a way to lower monthly premiums.
In 2026, the deductible for high-deductible versions of Plan G and Plan F is $2,950. Beneficiaries must pay this amount in covered medical costs before the policy begins paying benefits.
After the deductible is met, the coverage works similarly to the standard version of the plan.
High-deductible options are often selected by retirees who want strong protection against major medical expenses while keeping monthly costs lower.
Why Enrollment Timing Matters
The timing of Medigap enrollment plays a major role in whether beneficiaries can easily obtain coverage.
The most favorable enrollment window is the six-month Medigap Open Enrollment Period. This period begins when someone is both:
- 65 years old
- Enrolled in Medicare Part B
During this time, insurance companies must offer coverage regardless of health status. They cannot deny an application or increase premiums due to medical history.
After this enrollment window ends, insurers may review health records when evaluating applications. In some cases, companies may charge higher premiums or decline coverage.
Because of this rule, many new Medicare beneficiaries review Medigap options as soon as they become eligible.
Typical Benefits Provided by Medigap
While each plan offers different levels of coverage, most Medigap policies help with several common healthcare costs.
Typical benefits include:
- Part A hospital coinsurance for extended hospital stays
- Part B coinsurance for outpatient care
- Coverage for the first three pints of blood used in a medical procedure
- Skilled nursing facility coinsurance
- Hospice care coinsurance
Some plans also provide limited emergency medical coverage for healthcare received while traveling outside the United States.
These protections help reduce unexpected medical bills for retirees who rely on Original Medicare.
Insurance Companies Offering Medigap Policies
Many private insurance companies provide Medigap coverage across the United States. Major insurers offering these policies include:
- UnitedHealthcare
- Humana
- Aetna
- Blue Cross Blue Shield companies
- Mutual of Omaha
Even though plan benefits are standardized, monthly premiums can vary widely between companies. For this reason, many consumers compare multiple insurers before selecting a policy.
Medigap vs. Medicare Advantage: Key Differences
Medicare beneficiaries often compare Medigap with Medicare Advantage plans when deciding how to structure their healthcare coverage.
The two options differ in several important ways.
| Feature | Medigap with Original Medicare | Medicare Advantage |
|---|---|---|
| Doctor choice | Nationwide access to Medicare providers | Often limited to networks |
| Monthly premium | Usually higher | Often lower |
| Out-of-pocket predictability | Generally more predictable | Varies by plan |
| Additional benefits | Limited extras | Often includes dental or vision |
Medigap policies appeal to individuals who prefer flexibility in choosing doctors and hospitals throughout the United States.
Growing Demand for Supplemental Coverage
As Americans live longer and healthcare expenses continue rising, supplemental insurance remains a key part of retirement planning. Medigap coverage helps many retirees protect themselves from unexpected costs that could otherwise create financial stress.
For individuals who remain on Original Medicare, Medigap policies provide an added layer of security that helps make healthcare spending more predictable.
Choosing the Right Medigap Plan
Selecting the right Medigap policy involves comparing several factors, including:
- Monthly premiums
- Coverage level provided by each plan
- Personal healthcare needs
- Insurance company reputation
- Long-term affordability
Because benefits are standardized across insurers, many consumers focus on price and customer service when deciding which policy to purchase.
The Bottom Line
Medigap plans remain one of the most important tools for Medicare beneficiaries who want to control healthcare costs while keeping access to doctors nationwide. With Medicare expenses continuing to increase in 2026, supplemental coverage plays a major role in helping retirees manage medical spending during their later years.
What are your thoughts on Medigap coverage or Medicare supplements? Share your perspective in the comments and stay informed about future Medicare updates.