The low income subsidy medicare program continues to play a critical role in reducing prescription drug costs for millions of beneficiaries across the United States in 2026. Designed to lower financial barriers within Medicare Part D, this federal assistance program provides substantial relief for individuals with limited income and resources. As Medicare evolves under recent legislative reforms and cost-containment measures, the structure and operational impact of this subsidy remain central to health policy discussions, plan design strategies, and beneficiary access outcomes.
For policy professionals, healthcare administrators, and Medicare advisors, understanding the mechanics of this program is essential. It not only shapes prescription affordability but also influences enrollment trends, plan benchmarks, risk adjustment patterns, and state-federal coordination strategies. In today’s Medicare environment, where drug pricing reform and benefit restructuring continue to unfold, this subsidy stands as one of the most impactful affordability tools available within the federal health framework.
Program Foundation and Legislative Framework
The Medicare Part D Low-Income Subsidy, often referred to as Extra Help, was established alongside the creation of Medicare Part D prescription drug coverage. Its purpose was straightforward yet essential: ensure that individuals with limited financial means could access necessary medications without facing overwhelming out-of-pocket costs.
Since its launch in 2006, the program has undergone periodic adjustments to income thresholds, asset limits, and cost-sharing protections. More recently, federal policy expanded eligibility parameters to allow more beneficiaries to qualify for full benefits. These changes aligned the subsidy with broader affordability goals embedded in Medicare reform efforts. The updated income standards now allow individuals earning up to approximately 150 percent of the federal poverty level to qualify for comprehensive assistance, provided they meet resource requirements.
From a policy perspective, the program operates as a federal entitlement administered primarily through the Social Security Administration, while coordination with Medicare plan sponsors ensures cost-sharing reductions are applied in real time at the pharmacy counter.
Eligibility Criteria and Financial Thresholds
Eligibility for the subsidy is determined by two primary financial tests: income and countable resources. Beneficiaries must be entitled to Medicare Part A or enrolled in Medicare Part B. Income includes wages, Social Security benefits, pensions, and certain other forms of compensation. Some exclusions apply, depending on the type of income and household composition.
Resource limits cover liquid assets such as savings accounts, checking accounts, stocks, bonds, and certain additional property beyond a primary residence. A home, vehicle, personal belongings, and burial plots are typically excluded from countable resources. These exclusions prevent modest asset ownership from disqualifying otherwise eligible individuals.
Importantly, individuals who receive Supplemental Security Income, full Medicaid benefits, or participate in a Medicare Savings Program are generally deemed eligible automatically. This automatic qualification reduces administrative burden and ensures alignment across federal and state assistance programs.
For those not automatically enrolled, application through the Social Security Administration remains the primary pathway. Once approved, beneficiaries receive cost-sharing adjustments reflected directly in their Part D drug plan.
Benefit Structure and Cost Protections
The subsidy significantly reduces or eliminates key financial components of Medicare Part D. For eligible individuals, monthly drug plan premiums are either fully covered or reduced to benchmark levels. If a beneficiary selects a plan within the regional benchmark, no premium is owed. If the chosen plan exceeds the benchmark, the beneficiary pays only the difference.
Deductibles are either waived entirely or substantially lowered. This allows beneficiaries to begin accessing coverage immediately without meeting high upfront cost thresholds. Reduced copayments apply to both generic and brand-name medications, dramatically lowering out-of-pocket expenses at the pharmacy counter.
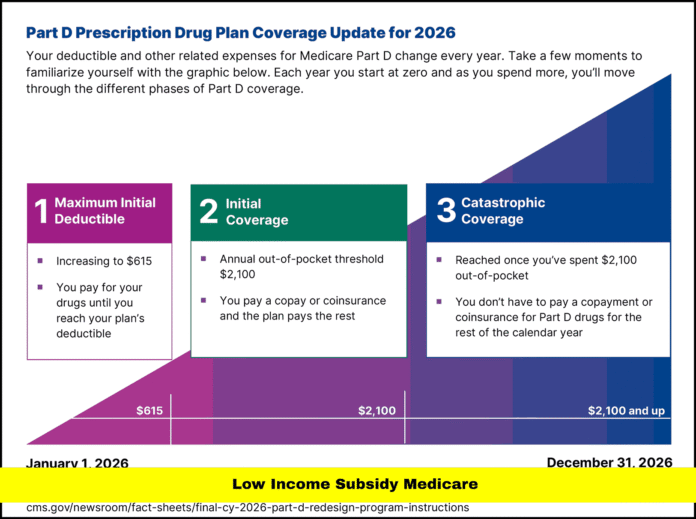
Another major protection involves catastrophic coverage. Once a beneficiary reaches the annual out-of-pocket limit defined by Medicare, cost sharing drops to zero for covered drugs for the remainder of the calendar year. This safeguard ensures that individuals with high medication needs are not exposed to unlimited financial liability.
Late enrollment penalties for Medicare Part D are also eliminated for subsidy recipients. This provision is particularly important for vulnerable populations who may have delayed enrollment due to confusion, hardship, or prior lack of awareness.
Interaction with Medicare Part D Redesign
Medicare Part D has undergone structural adjustments in recent years, particularly related to catastrophic thresholds and beneficiary spending caps. The subsidy operates within this redesigned framework, ensuring that cost protections remain aligned with new spending limits.
As Medicare phases in additional prescription drug affordability reforms, including annual out-of-pocket caps, the subsidy continues to function as a foundational support mechanism. It integrates seamlessly with benefit redesign provisions to preserve cost predictability for low-income beneficiaries.
For policy analysts, the integration between subsidy provisions and Part D redesign has implications for federal spending projections, actuarial modeling, and risk pool management. Subsidy enrollees represent a population with elevated prescription utilization, making plan payment structures and risk adjustment considerations particularly relevant.
Enrollment Flexibility and Special Enrollment Periods
One of the program’s most impactful features is the flexibility it grants beneficiaries to modify plan enrollment outside the standard annual enrollment window. Eligible individuals may change their Medicare Advantage or standalone drug plan more frequently than non-subsidy beneficiaries.
This monthly enrollment flexibility enhances consumer responsiveness. Beneficiaries can adjust plans if formularies change, preferred pharmacies shift, or medication needs evolve. Such flexibility improves alignment between coverage design and health status, reducing treatment interruptions.
Automatic enrollment mechanisms also protect individuals who qualify but have not selected a plan. In those cases, Medicare assigns beneficiaries to benchmark plans to ensure continuous prescription coverage. This safety measure reduces the risk of coverage gaps during eligibility transitions.
Coordination with State and Federal Assistance Programs
The subsidy does not operate in isolation. It intersects closely with Medicare Savings Programs administered by state Medicaid agencies. These programs assist with Part B premiums and, in some cases, cost sharing. When beneficiaries qualify for both programs, financial relief spans both medical and prescription coverage.
For dual-eligible individuals receiving Medicaid and Medicare, prescription cost sharing is effectively eliminated under the subsidy. This layered protection improves healthcare access and reduces financial strain among individuals with the lowest incomes.
Administrative coordination between federal and state agencies ensures that data sharing supports automatic enrollment processes. This alignment reduces redundant paperwork and accelerates benefit activation.
Impact on Medication Adherence and Health Outcomes
Research consistently shows that lowering out-of-pocket drug costs improves medication adherence. When financial barriers decrease, beneficiaries are more likely to fill prescriptions consistently and follow treatment regimens as prescribed.
The subsidy plays a direct role in addressing cost-related nonadherence. For chronic conditions such as diabetes, hypertension, and cardiovascular disease, uninterrupted access to medication can prevent hospitalizations and emergency interventions. This creates downstream cost savings within the broader Medicare system.
Health systems and accountable care organizations monitor adherence metrics closely. Subsidy participation correlates with improved pharmacy fill rates and reduced discontinuation rates for essential medications.
Administrative and Operational Considerations
From an administrative standpoint, the program requires precise coordination between Social Security, Medicare plan sponsors, pharmacy benefit managers, and pharmacies. Eligibility determinations must be transmitted accurately to ensure cost sharing reflects subsidy status in real time.
Plan sponsors incorporate subsidy enrollment projections into actuarial forecasts. Because beneficiaries receiving the subsidy often have higher medication utilization, accurate risk adjustment and payment calculations are essential to maintain plan stability.
Operational oversight also includes annual redetermination processes to confirm continued eligibility. Beneficiaries may need to update financial information to maintain subsidy status, depending on how they initially qualified.
Awareness Challenges and Outreach Efforts
Despite expanded eligibility thresholds, some individuals who qualify do not apply. Barriers include limited awareness, misconceptions about asset limits, or confusion about application procedures.
Outreach efforts target older adults, individuals with disabilities, and caregivers to improve enrollment rates. Clear communication about eligibility standards and benefit value remains a priority across federal and community organizations.
Increasing awareness improves equity in prescription access and strengthens the overall effectiveness of Medicare’s affordability initiatives.
Economic and Policy Implications
From a fiscal perspective, the subsidy represents a significant federal investment. However, policymakers view it as a cost-effective intervention that reduces more expensive healthcare utilization downstream. By preventing medication interruptions, the program contributes to lower hospitalization rates and improved disease management outcomes.
Actuarial modeling demonstrates that predictable prescription coverage for low-income beneficiaries stabilizes plan risk pools and supports broader market sustainability within Medicare Part D.
As healthcare inflation and drug pricing pressures persist, the subsidy remains central to federal efforts to shield vulnerable populations from disproportionate financial impact.
Looking Ahead: Sustainability and Future Policy Direction
While the program currently operates under expanded eligibility standards, ongoing policy discussions evaluate how best to sustain and optimize it. Topics include further streamlining enrollment, enhancing data integration, and expanding education efforts.
For professionals in healthcare policy and insurance design, monitoring the trajectory of this program is critical. It influences federal spending, beneficiary protection standards, and the competitive landscape among Part D plan sponsors.
The low income subsidy medicare framework stands as a stabilizing force within the Medicare ecosystem. It reduces disparities, supports medication adherence, and strengthens the financial foundation for millions of beneficiaries navigating prescription drug coverage.
Medicare affordability remains a central issue in American healthcare policy. As prescription drug costs continue to shape public discourse, programs designed to protect low-income beneficiaries will remain essential pillars of the system.
What are your thoughts on how Medicare affordability programs can evolve further to protect vulnerable populations? Share your perspective and stay informed on ongoing policy developments.